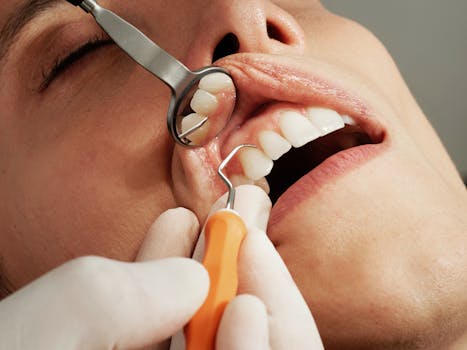
From diagnosis to therapy: the path to a cure for periodontitis
Periodontitis, often called periodontosis, is a serious disease of the periodontium caused by bacteria. It is an inflammation of the gums that, if left untreated, affects the jawbone and can lead to tooth loss. But don't worry, with the right knowledge and care you can keep your teeth and gums healthy.

What exactly is periodontitis?
Periodontitis is an inflammation of the periodontium caused by bacteria and can lead to symptoms such as bleeding gums, receding gums and bone loss. When the gums bleed, this is often the first sign of the onset of periodontitis. In the advanced stages, deeper gum pockets may develop where bacteria accumulate, further increasing inflammation.
Periodontitis often starts as gingivitis, a milder form of gum inflammation. If left untreated, it can develop into severe periodontitis, which affects the jawbone. The main cause of periodontitis is the bacterial plaque that constantly forms on the teeth. This plaque can become tartar, which can only be removed by professional teeth cleaning. Other risk factors may include smoking, diabetes mellitus, poor oral hygiene and genetic predisposition.
Symptoms and diagnosis
Symptoms of periodontitis include:
- Redness or swelling of the gums
- Bleeding gums
- Painful chewing
- Loosening of the teeth
- Recession of the gums
- Constant bad breath or halitosis
A dentist can determine if you have periodontitis by examining your mouth and taking x-rays. In particular, the depth of the gum pockets and the condition of the gum line will be checked.
Complications of periodontitis
In this section, we will highlight the potential complications of periodontitis.
- Tooth loss: One of the most serious complications of periodontitis is the loss of teeth, as the bone that supports the teeth is broken down by inflammation.
- Abscesses: Purulent abscesses can form in the gum pockets, causing pain and swelling.
- Gum recession: The gums can recede and expose the necks of the teeth, causing increased sensitivity.
- Jaw bone loss: Advanced bone loss can alter facial structure and affect appearance.
- Systemic effects: There is evidence that periodontitis may be associated with other health problems, including cardiovascular disease, diabetes and respiratory disease.
- Dental treatment complications: Bone loss can make placing implants or other dental procedures difficult.
- Spread of infection: In rare cases, the infection can enter the bloodstream and affect other parts of the body.
The role of periodontology
Periodontology is a speciality of dentistry that deals with the diagnosis, prevention and treatment of periodontal disease. In a specialised dental practice, patients receive comprehensive advice and treatment to improve the condition of the gums and periodontium.
The role of periodontology is vital as conditions such as periodontitis can not only lead to tooth loss, but are also associated with serious health problems. A periodontist has specialised knowledge and skills to treat complex and advanced cases of periodontal disease and often works across disciplines with other dental specialties to provide comprehensive care to patients.
The procedure of periodontitis therapy
Periodontal therapy begins with a thorough examination of the affected teeth and gums. Fillings, caries and other factors that may affect dental health are taken into account.
The therapy itself can take place in several steps:
- Medical history and diagnosis: A thorough examination is carried out before treatment begins. This includes questioning the patient about their oral care habits, a clinical examination of the mouth and X-rays to assess the condition of the jawbone.
- Professional dental cleaning: This involves removing plaque and tartar above and below the gum line. This is often the first step in reducing inflammation.
- Deep cleaning (scaling and root planing): If periodontitis is advanced, a deeper cleaning may be necessary. Special instruments, such as curettes, are used to remove plaque and calculus from the tooth surfaces and from the gum pockets. The roots of the teeth are smoothed to make it more difficult for bacteria to adhere. This is usually done under local anaesthetic.
- Drug treatment: In some cases, antibiotics or antimicrobial mouthwashes may be prescribed to fight the bacteria that cause periodontitis.
- Surgical procedures: In severe cases of periodontitis where previous treatments are not enough, surgical procedures may be necessary. This may involve removing diseased tissue, smoothing out bone defects or even bone augmentation procedures.
- Aftercare and regular check-ups: After treatment, regular check-ups and professional dental cleanings (often every 3-4 months) are necessary to ensure that periodontitis does not return and oral health is maintained.
- Oral hygiene: Patients are often educated to improve their oral hygiene, including proper brushing technique, flossing and mouth rinses.
Supportive periodontal therapy
Supportive periodontal therapy is an essential part of follow-up care after a completed periodontal treatment. Its main objective is to ensure the long-term treatment success of the previous therapy and to prevent a new outbreak of periodontitis. During the therapy, regular professional dental cleanings are performed, during which the gum pockets in particular are cleaned and monitored. In addition, patients are trained in optimal oral hygiene and educated about risk factors. Supportive periodontal therapy is thus a proactive approach to maintaining oral health at a stable level and minimising the risk of tooth loss due to the recurrence of periodontal disease.


For a healthy mouth and beautiful teeth, regular professional teeth cleaning is essential. Our specialists detect early signs of caries and prevent them.
- Personalised dental hygiene
- Gum check & caries control
- Painless cleaning with AIRFLOW
How can ALPINE WHITE help?
Although ALPINE WHITE does not currently offer periodontal treatment, we emphasise the importance of prevention. The treatment of periodontitis can vary depending on the severity and progress of the disease. So it is important to perform regular professional dental cleanings and maintain good oral hygiene to prevent the disease.
Our products are formulated to not only whiten your teeth but also support your overall oral health. Our Whitening Toothpaste Extra White and Whitening Toothpaste Sensitivity Relief are perfect for everyday dental care and to fight discolouration. They contain no harsh chemicals and are gentle enough for everyday use. Our Charcoal Powder is a natural product that helps to remove stubborn stains and restore the balance of the oral flora.
Also, come to our ALPINE WHITE studio for thorough dental hygiene. Dental hygiene not only helps you maintain your teeth but also ensures good overall health. Regular professional dental cleaning is important to maintain healthy gums, clean interdental spaces and prevent exposed necks of teeth.